Psoriasis is a chronic skin condition with several types. It’s considered an immune-mediated disease, meaning the immune system acts abnormally. It’s possible to have more than one type.
Psoriasis typically affects the skin, causing skin cells to build up faster than usual. It causes your skin to develop scaly patches that can be itchy and painful.
It can also affect other organ systems, especially the joints.
Psoriasis tends to appear pink or red on people with light or fair skin tones, with silvery-white scales. On medium skin tones, it can appear salmon-colored with silvery-white scales. On darker skin tones, psoriasis can look violet, brown, or reddish brown, often with light-colored or grayish-colored plaques.
There’s limited research and information about managing and diagnosing psoriasis in people of color. A
- White: 3.6%
- Black/African American: 1.9%
- Hispanic: 1.6%
These numbers may not tell the entire story, as people of color may be disproportionately undertreated and misdiagnosed. This is because psoriasis isn’t always recognized on skin of color.
Read on to learn more about the different types of psoriasis and how they’re treated.
The most common symptoms of psoriasis include:
- skin patches and scales that vary in color based on skin tone:
- red skin patches on light skin tones
- salmon-colored and silvery-white on medium skin tones
- violet, dark brown, or gray on darker skin tones
- scaly skin
- itchy skin
- joint swelling, stiffness, or pain, which are associated with psoriatic arthritis
The symptoms of psoriasis also vary based on the type of psoriasis you have. There are eight types of psoriasis:
- plaque
- guttate
- inverse
- pustular
- erythrodermic
- psoriatic arthritis
- nail
- scalp
Psoriasis isn’t contagious, regardless of type.
Psoriasis can also lead to mental stress, anxiety, and low self-esteem. Depression is also common in people who have psoriasis.
Other diseases have also been
There are also subcategories of psoriasis types. These appear differently depending on the location of the body.
Psoriasis patches on darker skin tones may also be more widespread, which can make it difficult to diagnose.
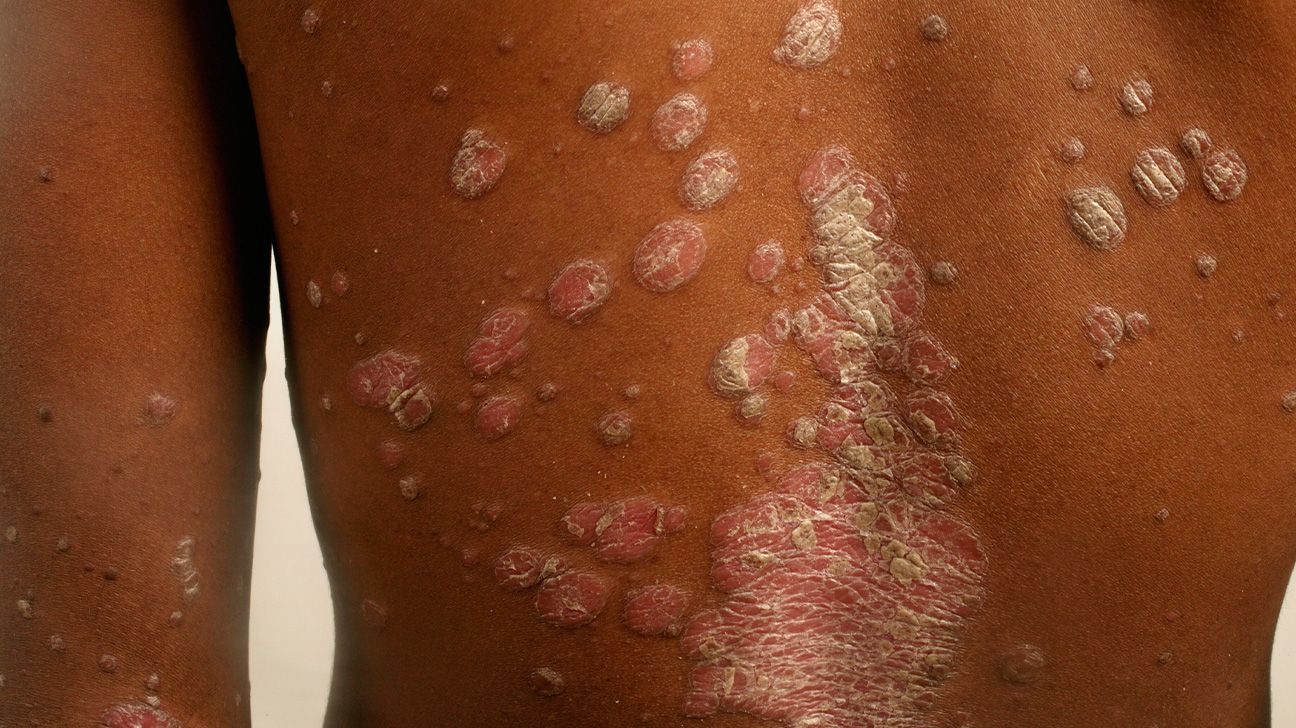
Plaque psoriasis, or psoriasis vulgaris, is the most common form of psoriasis. An estimated 80–90% of people diagnosed with psoriasis have plaque psoriasis.
This type is characterized by thick red or purplish patches of skin, often with silvery-white or gray scales. These patches often appear on your elbows, knees, lower back, or scalp.
Patches are usually 1 to 10 centimeters wide but can also be larger and cover more of your body. If you scratch at the scales, the symptoms will often get worse.
Treatments
As a way to ease discomfort, a doctor may recommend applying moisturizers to keep the skin from becoming too dry or irritated. These moisturizers include over-the-counter (OTC) cortisone creams or an ointment-based moisturizer.
A doctor may also work to identify your unique psoriasis triggers, including stress or lack of sleep.
Other treatments may include:
- vitamin D creams, such as calcipotriene (Dovonex) and calcitriol (Rocaltrol), to reduce the rate at which skin cells grow, in combination with topical steroids to reduce inflammation and itching
- topical retinoids, like tazarotene (Tazorac, Avage), to help reduce inflammation
- immunosuppressives, such as methotrexate or cyclosporine
- applications of coal tar, either by cream, oil, or shampoo
- biologics, a category of anti-inflammatory drugs
Medications may differ for guttate or erythrodermic psoriasis.
In some cases, you may need light therapy. This involves exposing the skin to both UVA and UVB rays. Sometimes, treatments combine prescription oral medications, light therapies, and prescription ointments to reduce inflammation.
With moderate to severe cases, you may be prescribed systemic medication in the form of oral, injectable, or intravenous (IV) medication.
Guttate psoriasis appears in small red spots on lighter skin tones. In darker skin tones, these spots may appear violet or brown.
Guttate is the second most common psoriasis type, affecting around 8% of people with psoriasis. Most of the time, it starts during childhood or young adulthood.
The spots are small, separate, and drop-shaped. They often appear on the torso and limbs, but they can also appear on your face and scalp. Spots are usually not as thick as plaque psoriasis, but they can develop into plaque psoriasis over time.
Guttate psoriasis usually begins after certain triggers. Triggers may include:
- strep throat
- stress
- skin injury
- infection
- medication
Treatments
To treat guttate psoriasis, a doctor may prescribe steroid creams, light therapy, and oral medications.
Determining the underlying cause of the infection can also help clear guttate psoriasis. If a bacterial infection is the cause, antibiotics may help.
Flexural or inverse psoriasis often appears in skinfolds, such as under the breasts, in the armpits, or around the groin. This type of psoriasis appears red or purple and is often shiny and smooth.
The sweat and moisture from skinfolds keep this form of psoriasis from shedding skin scales. Sometimes, it’s misdiagnosed as a fungal or bacterial infection. The skin-on-skin contact can make inverse psoriasis very uncomfortable.
Most people with inverse psoriasis also have a different form of psoriasis in other places on their body.
Treatments
The treatments for inverse psoriasis are similar to plaque psoriasis treatments. They can include:
- topical steroid creams
- nonsteroidal drugs such as phosphodiesterase (PDE)-4 inhibitor
- light therapy
- oral medications
- biologics, which are available via injection or IV infusion
A doctor may prescribe a lower-potency steroid cream to prevent your skin from thinning too much. You may also benefit from taking or applying medications that reduce yeast or bacteria growth.
Pustular psoriasis may be severe at times. This form of psoriasis may develop quickly in the form of many white pustules surrounded by red or darkened skin.
Pustular psoriasis may affect isolated areas of your body, like your hands and feet, or cover most of the skin’s surface. These pustules can also join together and form scaling. However, if it affects all areas of the body — such as the Von Zumbusch subtype — it
Some people experience cyclic periods of pustules and remission. While the pus is not infectious, this condition can cause flu-like symptoms such as:
- fever
- chills
- rapid pulse
- muscle weakness
- loss of appetite
There are three kinds of pustular psoriasis:
- von Zumbusch
- palmoplantar pustulosis
- acropustulosis
Each of the three forms of pustular psoriasis may have different symptoms and severity.
Treatments
Treatment may include OTC or prescription corticosteroid creams, oral medications, or light therapy. Biologics may also be recommended.
Identifying and treating the underlying cause may also help reduce reoccurrence of pustular psoriasis.
Erythrodermic psoriasis, or exfoliative psoriasis, is a rare type of psoriasis that looks bright red on lighter skin tones or dark purplish in people with darker skin tones. It also involves shedding of the skin.
This condition is a medical emergency. You may need to be hospitalized, as your body may not be able to manage your body temperature.
This form of psoriasis is widespread, with red or purple skin and silvery scales. It may cover large portions of your body. Exfoliation often occurs in larger pieces than the small scales typical to most psoriasis.
Erythrodermic psoriasis can develop from:
- pustular psoriasis
- widespread, poorly controlled plaque psoriasis
- a bad sunburn
- infection
- alcohol use disorder
- significant stress
- abrupt discontinuation of a systemic psoriasis medication
- using oral steroids, cyclosporin, or methotrexate
Treatments
Almost all cases of erythrodermic psoriasis will need to be treated at a hospital. There, you’ll receive a combination of therapies, which may include:
- an application of medicated wet dressings
- topical steroid applications
- biologics
- prescription oral medications
Reach out for medical advice immediately if you think you have erythrodermic psoriasis.
Psoriatic arthritis (PsA) is a painful and physically limiting condition that affects between 30% and 33% of people with psoriasis.
There are five subtypes of PsA with varying symptoms. There’s currently no cure for this condition.
Psoriasis is an autoimmune disease, so it can trigger your body to attack your joints and skin. It can affect many joints and often becomes quite severe in the hands, affecting the nails. Skin symptoms usually appear before joint symptoms.
Treatments
Treatments for psoriatic arthritis may include nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil) and naproxen sodium (Aleve). NSAIDs can help reduce the incidences of swelling and pain associated with psoriatic arthritis.
Prescription medications, such as an oral corticosteroid, may also help reduce inflammation that leads to psoriatic arthritis. Prescription topical medications used to treat PsA include:
- salicylic acid
- calcipotriene
- tazarotene
A unique category of medications known as disease-modifying antirheumatic drugs (DMARDs) can help reduce inflammation and joint damage. Biologics, which are a subcategory of DMARDs, may be prescribed to reduce inflammation at a cellular level.
Although not an official “type” of psoriasis, nail psoriasis is a common manifestation of psoriasis. It can often be confused with fungal infections and other infections of the nail.
Nail psoriasis can cause:
- nail pitting
- grooves
- discoloration
- loosening or crumbling of your nail
- thickened skin under your nail
- colored patches or spots under your nail
Sometimes, the nail can even crumble and fall off. There’s currently no cure for psoriatic nails, but some treatments may improve their health and appearance.
Treatments
Treatments for nail psoriasis are like the ones used for plaque psoriasis, but it may take time to see the effects of these treatments as nails grow very slowly.
Treatment options include:
- light therapy
- oral medications, such as methotrexate
- biologics
Scalp psoriasis is another manifestation that’s common in people with plaque psoriasis. For some people, it may cause severe dandruff. For others, it can be painful, itchy, and very noticeable at the hairline.
Scalp psoriasis can extend to your neck, face, and ears in one large patch or many smaller patches.
In some cases, scalp psoriasis can complicate regular hair hygiene. Excessive scratching can cause hair loss and scalp infections. The condition may also cause feelings of social stress.
Treatments
Topical treatments are most commonly used for scalp psoriasis. They may require an initial 2 months of intensive applications plus permanent, regular maintenance. Treatment options include:
- medicated shampoos
- tar preparations
- topical applications of vitamin D, known as calcipotriene (Dovonex)
Light therapy, oral medications, and biologics may also be recommended depending on the responsiveness to treatment.
There’s no one cure for any form of psoriasis, but remission and significant healing are possible. Your healthcare team can work with you to create a treatment plan that helps manage your condition. You can also take steps at home to manage psoriasis.
Home management includes:
- practicing relaxation techniques to reduce stress
- moisturizing dry skin
- quitting smoking
- avoiding products that irritate your skin
- wearing comfortable clothing that doesn’t rub the psoriasis
- eating a nutritious diet
Doctors may slowly build up to the most effective treatment plan for your psoriasis symptoms. Most start with a topical or light therapy treatment and only progress to systemic medications if the first line of treatment is unsuccessful.
Stress, anxiety, depression, and other mental health conditions can commonly occur in people with psoriasis. You may benefit from therapy or support groups where you can meet other people experiencing similar issues or concerns.
You can also talk with a healthcare professional about seeing a therapist who has experience with psoriasis. They will be able to help identify ways to cope that will work for you.
Visit the National Psoriasis Foundation for the latest information on research, events, and programs.
There are different types of psoriasis that present with different symptoms. While there’s currently no cure for psoriasis, treatments can help relieve and manage your symptoms.
The type of psoriasis you have and its severity will determine your treatment. Generally speaking, milder cases with smaller psoriasis patches can often be treated topically. More serious cases, with larger patches, may require systemic treatment.
Many people believe that psoriasis is contagious, but it will not spread from person to person. A combination of genetics, the environment, and immune system factors are believed to cause psoriasis.
Thanks to the advocacy work of dozens of psoriasis activists and organizations, psoriasis is gaining more support and awareness. Talk with a doctor if you believe you have psoriasis. They can provide treatment options and coping methods.









