Heberden nodes present as painful bumps on your finger joints. They’re a sign of osteoarthritis caused by the breakdown of joint cartilage. Treatments focus on pain relief.
People with osteoarthritis (OA) in their hands often develop bumps on their fingers known as Heberden nodes. These bumps are usually one of the most obvious signs of OA in the hands.
This article takes a closer look at Heberden nodes, including symptoms, causes, and treatments.
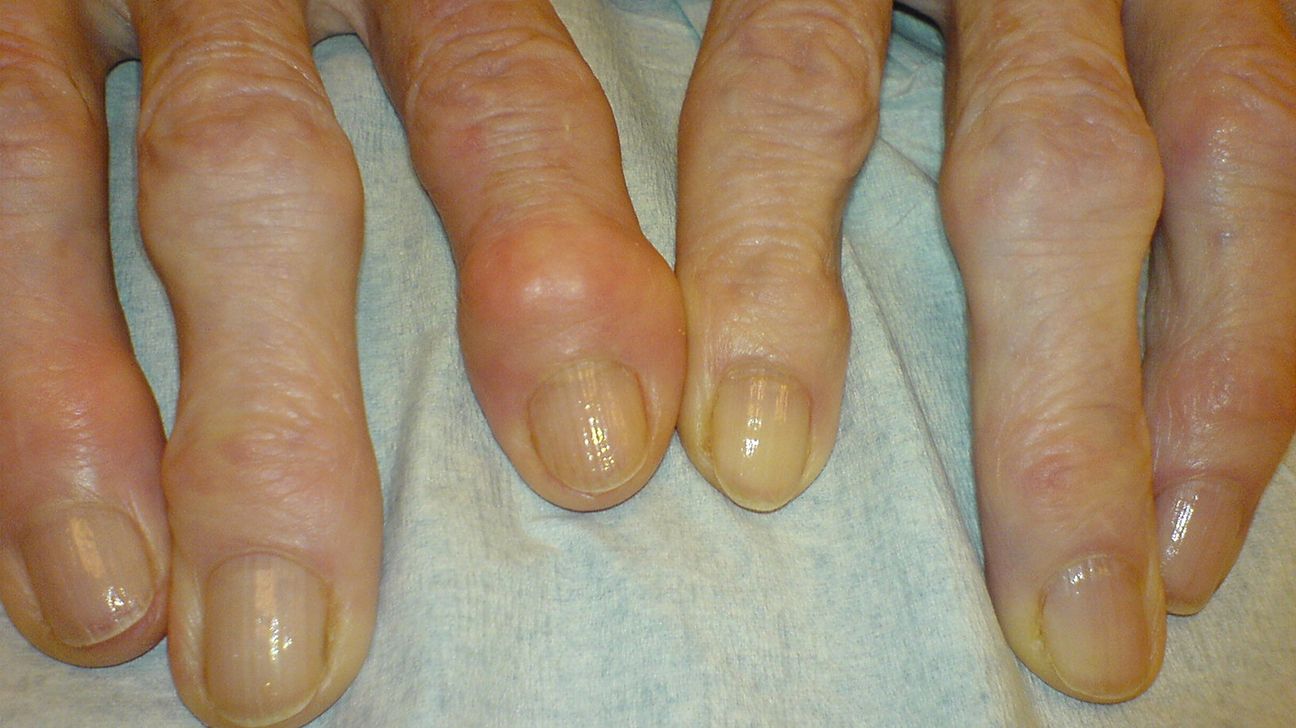
Heberden nodes are described as “bony swellings” that form on your hands due to osteoarthritis.
They’re named after physician William Heberden Sr., a doctor in the 1700s. He came up with the description of these swellings.
These firm growths occur on the finger joints nearest the fingertip, also called the distal interphalangeal joints.
Similar swellings located on the lower joints, or the proximal interphalangeal joints, are called Bouchard nodes.
Heberden nodes only develop in people who have OA.
The joints in your body, including the joints in your hands, all have a layer of cartilage that helps protect the bones. OA causes this cartilage to gradually erode. And without the protective layer of cartilage, the bones in your joints can grind against each other.
The bone-on-bone process can destroy existing bone and cause significant pain. As the cartilage continues to break down, your body reacts by growing new bone alongside the existing bone in the form of nodes or bony spurs. These growths can cause the fingers to become stiff and deformed.
Over time, the pain may lessen, but the deformity progresses.
Heberden nodes tend to appear after severe joint damage has already occurred, so they’re often seen as a marker of advanced OA, which is referred to as nodal OA.
If you have Heberden nodes, you can often see them by examining the end joints on your fingers.
Tiny firm-hard swellings may extend from the joint closest to your fingernail. In many cases, your fingers may twist or become crooked as the nodes form.
Common symptoms
Symptoms include:
- loss of motion
- pain
- swelling
- deformed and enlarged fingers
- stiffness
- weakness
Other defining features
Other defining features of Heberden nodes include the following.
- They can affect the fingers or thumb and are most common on the index and middle fingers.
- You may have more than one node on a finger.
- They can appear slowly or quickly.
- They’re often, but not always, painful when they begin to appear.
- For older women with gout and hypertension and taking a diuretic, such as hydrochlorothiazide, gout can deposit crystals in the nodes, causing acute inflammation. It’s a painful condition. The area may turn red and mimic an infection.
Some cases of Heberden nodes may be asymptomatic or only cause mild or few symptoms.
Effect on daily life
If you have Heberden nodes, you may have difficulty performing tasks that require gripping or pinching like turning the key in your car’s ignition or uncapping a soda bottle.
You may feel limited in your daily activities, and it may be hard to complete tasks for work or household chores.
This can affect your quality of life. For some people, it could even lead to the development of mental health disorders, such as depression and anxiety.
Osteoarthritis is the most common type of arthritis. It often affects older people, but over half of those who have both OA and Heberden nodes receive a diagnosis before age 65 years.
Other risk factors include:
- hereditary conditions that affect the joints
- having OA in the knee or elsewhere in the body
- rheumatoid arthritis, which can cause joint and cartilage changes
- gout, which can affect periarticular bony erosion
- having a family history of these nodes
- having obesity, as this
may increase the risk of OA,including hand osteoarthritis - doing sports or jobs that involve repetitive movements
There’s no specific treatment for Heberden nodes. Options for relieving pain may include:
- topical treatments containing capsaicin or nonsteroidal anti-inflammatory drugs (NSAIDs), which are usually given during the acute (painful) phase.
- applying heat and cold pads to reduce pain and inflammation
- splint devices (orthoses) aimed to support specific finger joints
- steroid injections, which may be difficult to give in this type of joint, according to one expert, but anesthetizing the skin, with a cold spray, for example, and using a very small needle can help a person better tolerate the injection
- surgery to fuse the joints if symptoms are severe and other options have not worked
In one small
However, more research is necessary to identify the best ways to deliver this procedure and examine the long-term effects.
Lifestyle choices
Experts from the
Options may include:
- Occupational therapy (OT), and the subspecialty hand OT: OT helps you learn new ways of using your hands. Hand OT analyzes your hand function to determine the best methods to benefit your situation. Examples of these methods may include splits, specific exercise programs, and assistive devices.
- Physical therapy (PT): PT helps to enhance or maintain mobility.
- Cognitive behavioral therapy (CBT): CBT helps you develop methods for managing ongoing pain, sleep, and stress-related issues.
Some people with OA find that using elastic “arthritis gloves” with open fingertips is helpful for increasing their hand mobility.
Experts recommend exercise for everyone with OA, including Heberden nodes.
Staying active can help improve overall strength and flexibility, and it may help manage stress and anxiety. Specific exercises may help keep your fingers mobile.
Medications
Over-the-counter medications include:
- NSAIDs, such as ibuprofen, for relieving pain and inflammation
- acetaminophen, for pain
- creams and ointments containing capsaicin or NSAIDs
If these do not work, your healthcare professional may prescribe:
- higher dose NSAIDs
- duloxetine (Cymbalta)
- corticosteroid injections if appropriate
Occasionally antidepressants may be prescribed to help relieve stress, anxiety, and depression, which can occur with many chronic conditions.
Alternative therapies
Other home and alternative therapies include:
- acupuncture
- paraffin, which is a type of heat therapy
- gloves that are designed to be warmed, such as those that can be warmed in a microwave
- soaking hands in a solution of warm water and magnesium salts
- wrapping a warm towel (warmed in the microwave or in warm water) around your hand
There’s
Surgery (a rare option)
Surgical treatment is rarely done and is usually a last resort after conventional treatment options have proven unsuccessful.
Joint replacement surgery is common in knee and hip OA. However, it’s not commonly done for arthritis of the fingers or thumbs, as this specific surgical procedure has a low success rate.
Treatment options to avoid
People sometimes use the following supplements for osteoarthritis, but the
- fish oil
- vitamin D
- glucosamine
- chondroitin sulfate
If you’re experiencing pain, swelling, and a loss of motion in your fingers, it’s a good idea to see a doctor. They will:
- ask you about your symptoms
- request and assess your medical history and medications
- give you a physical exam
- in some cases, recommend imaging tests or lab tests
If your doctor confirms an OA diagnosis, they’ll work with you to create a treatment plan that works best for you.
