Immunocompromised? Here’s How to Navigate the Ever-Changing COVID-19 Guidelines
August 23, 2021
Content created for the Bezzy community and sponsored by our partners. Learn More
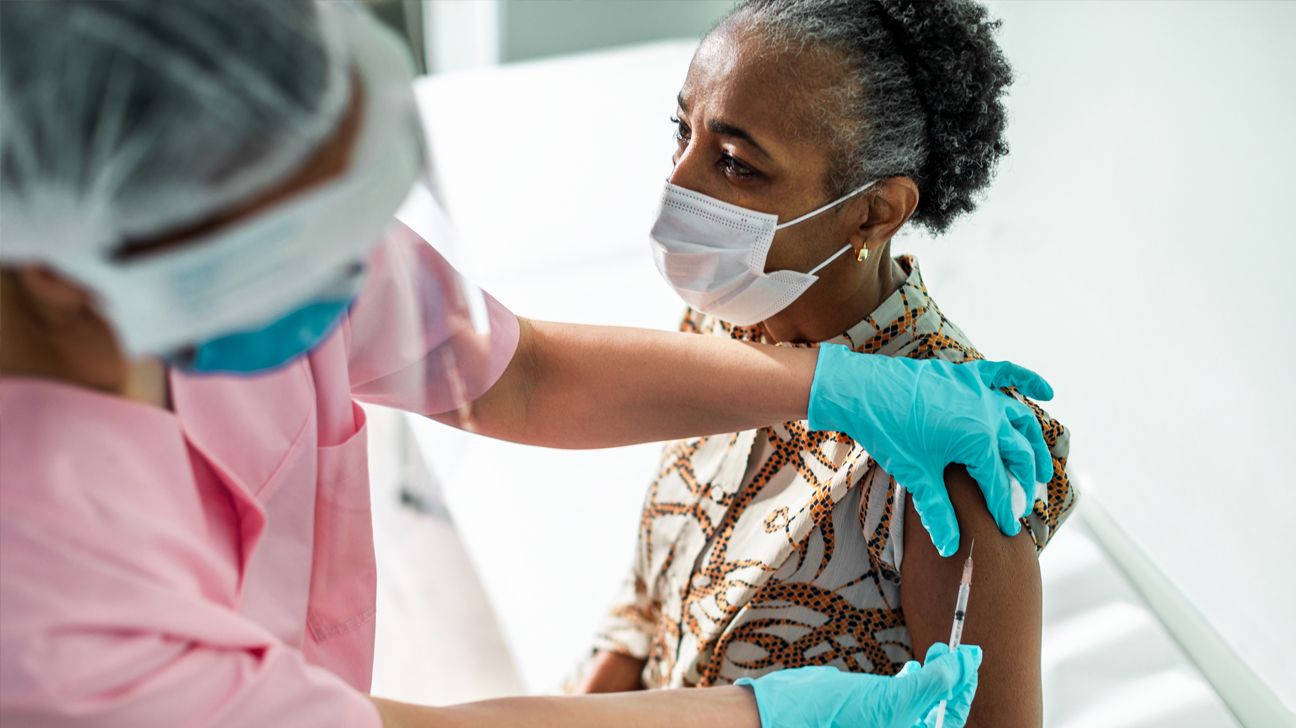
Marko Geber/Getty Images
Understanding our unique set of concerns and protocols can feel dizzying. But there are actions you can take to protect yourself.
I still remember the somewhat frantic phone call I placed to my rheumatologist in March of 2020. I had started hearing the phrase “those with compromised immune systems” in the news. It was a phrase meant to calm the general public — don’t worry, this doesn’t apply to you — except in my case, it did.
For years now, I’ve been on a biologic medication that keeps my autoimmune disease, psoriatic arthritis (PsA), in check. Since my disease is rooted in an overactive immune system, the medicine is designed to suppress part of that immune response.
In my case, the medicine is extremely well-targeted, and my overall immune function is generally normal. But I worried. Did I really want to be using medication to suppress my immune system right now?
“Don’t go off your medication,” my doctor advised. “But take precautions. You don’t want to get this thing.”
The reality is, immunocompromised people have a unique set of concerns and protocols when it comes to preventing and treating COVID-19.
A lot of research has been done, and is still being done, to understand just how this virus and disease affect those with impaired immune function.
For example, a 2021 study of transplant patients found that immunocompromised people may not have developed the same level of antibodies as people who are not immunocompromised due to their initial doses of COVID-19 vaccine. (It’s important to note that while antibodies may be a marker of protection against the coronavirus, they are only one piece of a complicated puzzle.)
Also, once they’ve contracted the coronavirus, immunocompromised adults may have a harder time fighting COVID-19 and have higher rates of hospitalization than the general population.
From vaccines to mask mandates to social distancing, here are some tips from experts on how to navigate this somewhat dizzying set of concerns.


Talk to your doctor
“Careful conversations with your healthcare provider are very important,” says Balazs Halmos, MD, an oncologist at Montefiore Medical Center in Bronx, New York.
Especially when it comes to people who are immunocompromised, there is no one-size-fits-all approach. Specific recommendations may be based on the medications you’re on, underlying diseases or conditions, your age, and other details.
It’s important to speak to your healthcare team to understand how the changing COVID-19 landscape affects you personally.
Consider a third vaccine dose
For many immunocompromised people, a supplemental dose of vaccine is now authorized by the Food and Drug Administration (FDA) and recommended by the Centers for Disease Control and Prevention (CDC).
Per the CDC recommendations, this group includes but is not limited to people currently undergoing or who recently received cancer treatment, solid organ or stem cell transplant recipients, people with advanced or untreated HIV, and people on immunosuppressive medications, including high dose steroids.
If you initially received one of the mRNA vaccines (Pfizer-BioNTech or Moderna) and are moderately to severely immunocompromised, the CDC recommends a third dose of the same vaccine. (If you initially received the single-dose Johnson & Johnson vaccine, no recommendation for additional doses has been approved yet.)
Both CVS and Walgreens pharmacies are already making these supplemental doses available. Be sure the pharmacy is offering the same vaccine you initially received.
Local health departments are expected to be rolling out administration of these additional doses soon. As always, check with your doctor to make sure a supplemental dose is appropriate for your specific medical condition.
Act unvaccinated
“Get vaccinated, act unvaccinated.”
This is the mantra Dorry Segev, MD, PhD, a professor of surgery at Johns Hopkins University School of Medicine and professor of epidemiology at Johns Hopkins Bloomberg School of Public Health, has been repeating to his patients since the vaccines first became available. (He’s been leading an observational study of COVID-19 vaccine responses in immunosuppressed people since December 2020.)
Immunocompromised people should continue wearing masks indoors, maintaining a 6-foot distance from those outside their households, and avoiding crowds, even after vaccination and regardless of local mandates.
All of the same precautions that most people were taking at the peak of pandemic compliance, including avoiding unnecessary errands and using hand sanitizer, may continue to be appropriate for immunocompromised people until the pandemic is truly over.
Contact your doctor after an exposure
Monoclonal antibody treatment (the treatment given to former President Donald Trump after he contracted the coronavirus in 2020) may help prevent severe illness, especially in vulnerable patients.
What has not been as well publicized is that the FDA has authorized the use of monoclonal antibody treatment prophylactically in immunocompromised individuals who have been exposed to the virus.
Administering these antibodies before symptoms even develop may act as an additional boost to the immune system, preventing the development of symptomatic disease.
This treatment, which won’t be appropriate for everyone, must be timely to be effective, so be sure to reach out to your healthcare provider as soon as you become aware of a known exposure.
Don’t rely on antibody testing
If you’re immunocompromised, you may be wondering whether your body was able to mount a sufficient immune response to the COVID-19 vaccine. It can be tempting, given the existence of antibody testing, to try to use this as an indicator of immunity.
However, both Segev and Halmos caution against the idea of using antibody testing alone to gauge immunity. Antibodies are only one part of the immune picture.
Even with a high level of antibodies, if someone has a blunted T-cell response, for example, their functional immunity may still be low. Those who find they have a high level of antibodies may end up with a false sense of security.
Antibody testing might be appropriate if, for example, you are being called back to work in a risky environment and you need a data point to prove that you are not as protected by vaccination as the general population, shares Segev. In a small number of patients for whom vaccination may carry its own risk, antibody testing can reveal whether a supplemental vaccine dose is even necessary, he adds.
As with most things, it’s a good idea to talk with your doctor about the benefits and drawbacks for you.
The takeaway
In general, for most immunocompromised people, it is best to assume you are less protected than the general population.
This makes it all the more important for the general population to do their part in ending this pandemic by getting vaccinated, masking around potentially vulnerable individuals, and following CDC guidelines.
Article originally appeared on August 23, 2021 on Bezzy’s sister site, Healthline. Last medically reviewed on August 23, 2021.
Medically reviewed on August 23, 2021
8 Sources


Like the story? React, bookmark, or share below:
Have thoughts or suggestions about this article? Email us at article-feedback@bezzy.com.
About the author